Below is a compilation table of the cellular constituents that can be seen in urine. Note, that the magnification is not equal for these images.
| Cell | Identification | Interpretation |
RBC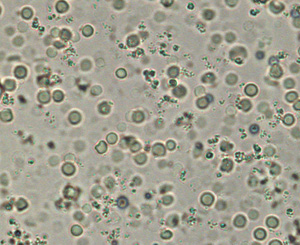 Fig 1: RBC and amorphous crystals Fig 1: RBC and amorphous crystals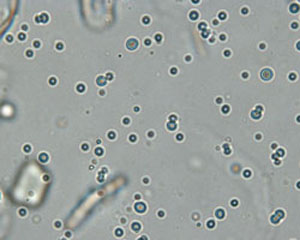 Fig 2: Fat droplets Fig 2: Fat droplets |
Round, slightly red-tinged, smooth textured cells, which may be biconcave in fresh urine. May be spiky (crenated) in stored urine | Classified as number per HPF: none seen, <5, 5-20, 20-100, or >100Normal: Up to 5 RBC/HPF generally are considered acceptable for “normal” urine. May lyse in very alkaline or dilute (USG < 1.008) urineCompared to fat droplets: RBC are more uniform and red-tinged versus fat droplets are more variable in shape, slightly greenish-tinged (or refractile), have a darker edge, are more globular shape (this can be visualized when you focus up and down) and usually float to the top of the coverslip (thus when fat droplets are in focus, the other urine constituents are out of focus – see Fig 2) |
WBC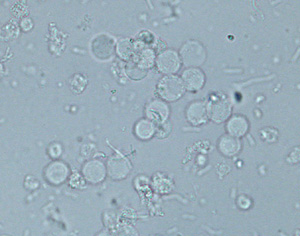 Fig 3: WBC and bacteria Fig 3: WBC and bacteria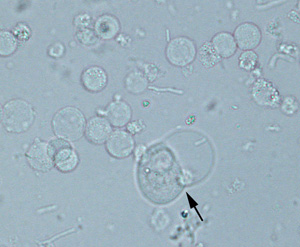 Fig 4: WBC and transitional epithelial cell (arrow) Fig 4: WBC and transitional epithelial cell (arrow) |
Round, colorless cells with a grainy texture (see Fig 3 – bacterial rods are also visible in the background), may see nuclei of cells | Classified as number per HPF: none seen, <5, 5-20, 20-100, or >100Normal: Up to 5 WBC/HPF generally are considered acceptable for “normal” urine – these are normally segmented neutrophils. May lyse in very alkaline or dilute (USG < 1.008) urineCompared to RBC: WBC are more grainy and largerCompared to transitional epithelial cells: WBC are smaller with rounder borders than epithelial cells which vary in size, are less grainy and usually have eccentric nuclei (when visible) (see arrowed cell Fig 4, which is from the same urine as Fig 3). |
Transitional epithelial cell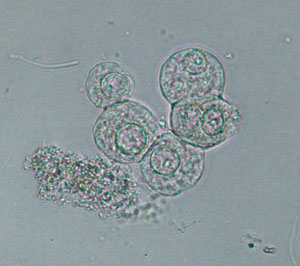 Fig 5: Transitional epithelial cell Fig 5: Transitional epithelial cell |
Variable size and shape (depends on origin): round or polygonal, pear-shaped, caudate (pelvis), tailed, spindle, may develop refractile, fatty inclusions with storage | From renal pelvis, ureters, urinary bladder and/or urethra.Compared to WBC: WBC are smaller and more uniformly roundCompared to squamous epithelial cells: Transitional cells are smaller with rounder (not as angular) borders. Can be seen in normal urine (few in samples collected by mid-stream catch or cystocentesis, more in catheterized specimens due to catheter-induced sloughing) as single cells or small clusters, more may exfoliate with inflammation. Difficult to distinguish from neoplastic cells – this requires urine cytology |
Squamous epithelial cell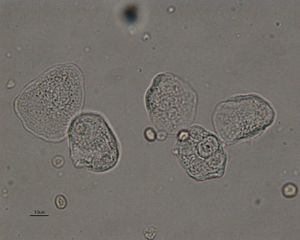 Fig 6: Squamous epithelial cells Fig 6: Squamous epithelial cells |
Largest cell in urine (Fig 6 was taken at lower magnification than the other images on this page). Thin, flat cells, with angular borders, anuclear or small central nucleus, present as single cells (Fig 6) or in variably-sized sheets | Represent contamination (from skin, genital tract, prepuce in male dogs) in voided urine or may reflect squamous metaplasia of prostate (from exogenous estrogen or an estrogen-secreting Sertoli cell tumor) especially if in large numbers |
Neoplasia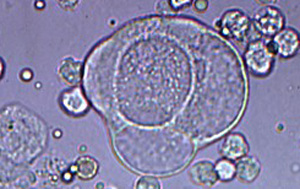 Fig 7: Neoplastic cell Fig 7: Neoplastic cell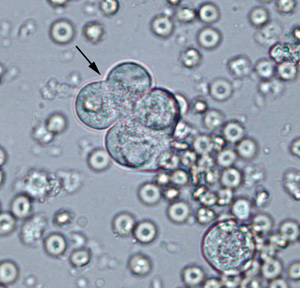 Fig 8: Neoplastic cell (arrow) and RBC Fig 8: Neoplastic cell (arrow) and RBC |
Frequently exfoliate as variably sized irregular clusters. | May exfoliate into urine in animals with tumors of the genitourinary tract. Most common type is transitional cell carcinoma (TCC) – arises in urinary bladder, urethra (including prostatic urethra in dogs). Rarely, lymphomas and renal carcinomas can also be observed in urine sedimentsCompared to normal transitional epithelial cells: Display cytologic criteria of malignancy such as variation in cell and nuclear size (Fig 7). Abnormal features may be difficult to discern in unstained urine sediments, particularly in stored samples where nuclei and cells swell with time. For instance, compare the cluster of neoplastic transitional epithelial cells (arrow in Fig 8) to the normal transitional epithelial cells demonstrated in Fig 5. The cells look quite similar. In these cases, cytologic examination of a Wright’s (or Diff-quik-stained) urine sediment is the preferred method of diagnosis |
